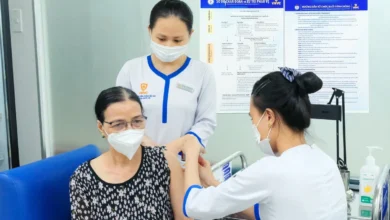
Understanding the Role of Blood Tests and Early Detection in Breast Cancer Management: Insights from the International Breast Cancer Symposium 2026

The International Breast Cancer Symposium 2026, held in Hanoi from April 22 to 23, has brought together leading oncologists, researchers, and medical professionals to address the evolving landscape of breast cancer treatment and diagnosis in Vietnam. During the event, Associate Professor Dr. Le Hong Quang, Head of the Breast Surgery Department at K Hospital—Vietnam’s leading oncology center—provided critical updates on the state of the disease within the country. According to Dr. Quang, Vietnam records approximately 25,000 new cases of breast cancer annually. However, there is a significant silver lining: due to advancements in early detection and the implementation of standardized treatment protocols, the five-year survival rate for breast cancer patients in Vietnam has reached an impressive 85% to 90%. This statistic underscores a major shift in the national healthcare outcome, with many patients living long, high-quality lives for 30 years or more following their initial diagnosis.
A Decisive Shift in Diagnosis Timelines
One of the most profound changes highlighted at the symposium is the transition in how and when patients seek medical intervention. Dr. Quang noted that 15 to 20 years ago, the majority of breast cancer cases in Vietnam were diagnosed at advanced stages. Specifically, about three-quarters of patients arrived at hospitals when the disease had already progressed significantly, limiting treatment options and reducing the likelihood of long-term survival. Today, that ratio has effectively been reversed. Through consistent public health education programs and enhanced media communication regarding women’s health, approximately 75% of patients now seek medical consultation and screening at an early stage.
This shift is not merely a statistical curiosity but a fundamental change in the clinical reality of oncology in Southeast Asia. Early detection allows for breast-conserving surgeries and less aggressive systemic therapies, which not only improve survival rates but also enhance the psychological and physical well-being of survivors. The symposium emphasized that this progress is the result of a multi-decade effort to de-stigmatize cancer and encourage proactive health-seeking behavior among the Vietnamese population.
Debunking the Misconceptions of Cancer Marker Blood Tests
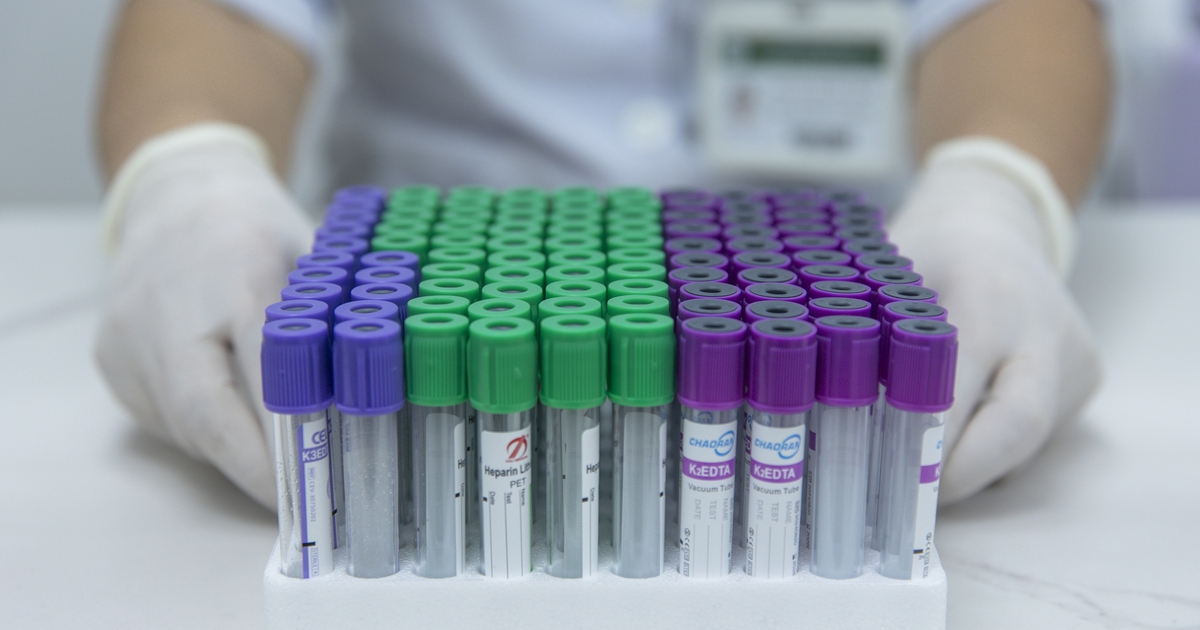
A major point of discussion at the 2026 symposium was the widespread misunderstanding regarding blood tests used to identify "cancer markers" (also known as tumor markers). As diagnostic technology becomes more accessible, many individuals have turned to independent blood tests in hopes of a quick confirmation of their health status. Dr. Quang issued a stern warning against the over-reliance on these single-index markers.
"A standalone marker test cannot be used as a definitive indicator of cancer," Dr. Quang explained. He noted that relying on a single elevated index often leads to unnecessary anxiety and psychological distress for patients. In clinical practice, cancer markers like CA 15-3 (often associated with breast cancer) can be elevated due to various non-cancerous conditions, including inflammation, benign cysts, or even certain lifestyle factors. Conversely, some patients with early-stage cancer may show normal marker levels, leading to a dangerous false sense of security.
The consensus among experts at the Hanoi event was clear: a professional diagnosis must be a synthesis of clinical examination, advanced imaging (such as mammography or ultrasound), and, where necessary, histopathology (biopsy). Blood markers are primarily useful for monitoring a patient’s response to treatment or detecting a recurrence in someone already diagnosed, rather than as a primary tool for initial screening in the general population.
The Integration of Artificial Intelligence in Modern Oncology
The International Breast Cancer Symposium 2026 also served as a platform to showcase the integration of high-tech solutions in the fight against cancer. Artificial Intelligence (AI) has emerged as a powerful ally for Vietnamese oncologists. Dr. Quang detailed how AI is currently being utilized to assist doctors in evaluating diagnostic images with higher precision and synthesizing vast amounts of global data to tailor treatment protocols.
By processing information from multiple international sources, AI helps multi-disciplinary teams (MDTs) conduct more effective consultations. It allows for "personalized medicine," where the treatment plan is specifically optimized for the unique genetic and biological profile of an individual’s tumor. However, Dr. Quang emphasized a critical boundary: "AI is a tool for support, data searching, and analysis to save time. The physician remains the final decision-maker, bearing the ultimate ethical and legal responsibility for the patient’s diagnosis and treatment path."
This human-centric approach to AI ensures that while technology improves efficiency, the nuances of patient care—such as empathy, ethical considerations, and complex clinical judgment—remain in the hands of qualified medical professionals.
Comprehensive Treatment Modalities and Global Integration
Vietnam’s approach to breast cancer has rapidly aligned with international standards, particularly in the realm of multi-modal therapy. The symposium highlighted that the treatment of breast cancer is no longer just about surgery. It involves a sophisticated combination of:
- Advanced Surgery: Moving toward breast-conserving techniques and oncoplastic surgery to maintain the patient’s physical appearance.
- Targeted Therapy: Using drugs designed to "target" specific molecules involved in the growth and spread of cancer cells, which minimizes damage to healthy cells.
- Immunotherapy: Bolstering the patient’s own immune system to recognize and destroy cancer cells.
- Advanced Radiotherapy: Utilizing precise techniques to target tumors while sparing surrounding healthy tissue like the heart and lungs.
- Molecular Diagnostics: This includes genetic testing (such as BRCA1 and BRCA2 mutations) and immunohistochemistry (IHC) to classify breast cancer into subtypes (e.g., HER2-positive, Triple Negative, or Hormone Receptor-positive).
These advancements allow doctors to move away from a "one-size-fits-all" approach. By understanding the molecular subtype of the cancer, Vietnamese doctors can prescribe the most effective medication from the outset, significantly improving the prognosis.
Recognizing Early Warning Signs and the Importance of Screening
Despite the technological leaps, the symposium concluded that the most effective tool against breast cancer remains the awareness of the individual. Dr. Quang and his colleagues reiterated the importance of annual screenings for women, particularly those aged 40 and older. For those with a family history of the disease, screening should often begin even earlier.
The medical community at the event outlined several "red flag" symptoms that necessitate an immediate visit to a specialist:
- Presence of Lumps: Any unusual hard masses or thickening in the breast or underarm area.
- Size and Shape Discrepancies: A noticeable increase in the size of one breast that is not related to the menstrual cycle, or a lack of symmetry between the two breasts.
- Skin Changes: Redness, swelling, or a "peau d’orange" (orange peel) texture on the skin of the breast.
- Nipple Abnormalities: Nipple retraction (turning inward), discharge other than breast milk, or skin that becomes scaly, red, or crusted around the nipple area.
- Persistent Pain: While breast cancer is often painless in its early stages, any persistent, localized pain should be investigated.
Analysis of Implications for Vietnam’s Healthcare System
The data presented at the International Breast Cancer Symposium 2026 reflects a broader success story in Vietnam’s public health strategy. The increase in the five-year survival rate to 90% is a testament to the effectiveness of the National Cancer Control Program. However, the rise to 25,000 new cases annually also signals a growing burden on the healthcare infrastructure.
The emphasis on early detection is not only a matter of saving lives but also an economic necessity. Treating early-stage breast cancer is significantly less expensive than managing metastatic disease, which requires long-term, high-cost biological and targeted therapies. By shifting the bulk of diagnoses to the early stages, the Vietnamese healthcare system can allocate resources more efficiently.
Furthermore, the warning regarding "cancer markers" serves as an important call for better regulation and public communication regarding "check-up packages" offered by private clinics. Ensuring that the public understands the limitations of blood tests prevents the waste of financial resources and mitigates unnecessary psychological trauma.
As the symposium wrapped up, the message was clear: the combination of a proactive public, technologically empowered doctors, and a robust multi-modal treatment framework has turned breast cancer from a "death sentence" into a manageable, and often curable, chronic condition in Vietnam. The continued focus on international collaboration and the adoption of cutting-edge technology like AI and molecular testing will be the pillars of oncology in the years to come, ensuring that the survival rates continue to climb toward the goal of total eradication of late-stage mortality.